The Complexities of Cholesterol
 Did you know that approximately 50% of Americans who suffered heart attacks had “normal cholesterol numbers” as reported by The National Heart, Lung and Blood Institute. Traditional testing that measures the total concentration of cholesterol (Total Cholesterol, HDL {good} cholesterol and LDL {bad} cholesterol), has historically been used as the key indicator for cardiovascular disease risk may not provide an accurate assessment according to the National Cholesterol Education Program.
Did you know that approximately 50% of Americans who suffered heart attacks had “normal cholesterol numbers” as reported by The National Heart, Lung and Blood Institute. Traditional testing that measures the total concentration of cholesterol (Total Cholesterol, HDL {good} cholesterol and LDL {bad} cholesterol), has historically been used as the key indicator for cardiovascular disease risk may not provide an accurate assessment according to the National Cholesterol Education Program.
Measuring the number and size of cholesterol-carrying particles, called lipoproteins (as well as inflammatory markers and other metabolic indicators), has been shown to be more important for interpreting the risk of heart disease.
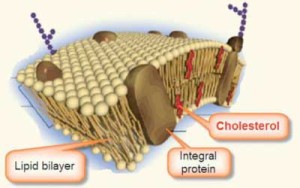
Lipoproteins are molecules that transport cholesterol through the blood. There are large and small sized lipoproteins.
To illustrate, think of t

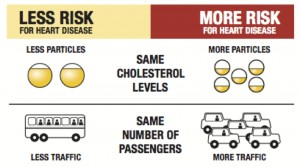

The number and size of the vehicles on the road determines whether there is increased risk of a traffic jam, not the number of people traveling in the vehicles. The higher the count of small-sized lipoprotein particles (cars), the higher the risk of cardiovascular disease. Understanding your lipoprotein status is essential for determining both your risk as well as the most appropriate, targeted intervention for your body.
Last year, nearly 21 million Americans were prescribed cholesterol-lowering medications, yet, cholesterol is actually a crucial element in the body necessary for brain cells, cell membranes and hormone balance. If cholesterol is so essential, how did we come to demonize it? In the 1950’s pathologists searching for the cause of heart disease discovered that blood vessels of heart disease patients were often clogged with plaque and debris. Cholesterol was at the mushy center of this plaque and was thought to be the cause of the disease. For decades since then, the avoidance of fat intake has been prescribed, however it has not led to decreased cholesterol levels or a reduction in cardiovascular risk. In fact, data suggests the opposite.



Low fat diets often incorporate more calories from the carbohydrate category that can elevate our blood sugar more quickly and actually contribute to increased cholesterol levels and damage to the lining of the arteries. Imbalances in food intake have also been shown to lead to the development of other chronic conditions such as Type II Diabetes, inflammation and obesity. Understanding how your body responds to different food combinations can have a dramatic effect on reducing your cardiometabolic risk.




There are additional factors and nuances that affect cholesterol and heart disease risk than are specific to you. Whether you are dealing with cholesterol issues, or have other health concerns, we can help you examine your situation and genetic attributes to help you select, and implement, the most appropriate course of action for you.

